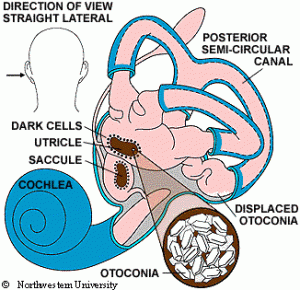
Muscle Power and Fall Risk
https://dynamicmobilitypt.com/wp-content/themes/osmosis/images/empty/thumbnail.jpg 150 150 Tonya Fuller Tonya Fuller https://secure.gravatar.com/avatar/bfa0f6df0b783409ca9fbb55d0f6b461?s=96&d=mm&r=g20 – 35% of older adults report falling once per year. Being white, having a higher body fat mass, smoking, higher use of alcohol, hip/joint pain, higher cognitive functioning, history of a fall, high blood pressure, history of heart attack or stroke, 4 or more medications, and poor physical performance were linked to older adults with fall injuries. Other conditions such as, osteoarthritis, diabetes, and heart disease have been related to lower leg muscle function. Age related changes can reduce muscle function including strength and power.
Muscle Power and Fall Risk:
A recent study suggests that muscle power can be a great indicator for fall risk in older adults. But what is muscle power? Muscle power differs from strength in that power adds a component of speed. It can be described as the amount of force you can generate over a short period of time. So it really relates to your ability to take a quick step to catch yourself if you trip on a crack in the sidewalk, for example. We need to be able to make those quick movements to prevent falls from happening. In this study, higher leg power was related to an 18% lower fall risk over 4.5 years in community dwelling men.
How can I train power to prevent falls and stay safe?
The best way to avoid falls is to be proactive in your training to improve balance, strength, and power. There are a number of different ways that older adults can add in exercise to improve muscle power, and therefore prevent future falls. The simplest way is to add speed to exercises at home or with any exercise program. This can be as simple as doing squats, heel raises, or lunges and just focusing on a quick movement up, and controlling the movement back down.

There has also been research to suggest that adding unstable surfaces with resistance training can improve power, as well as overall balance. So with those same squats, heel raises, and lunges adding a foam pad, a pillow, or a Bosu ball under the feet can improve power.
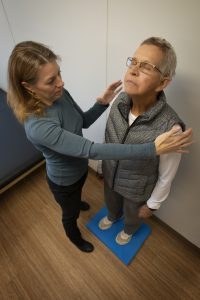

For more ideas of exercises, follow us on social media at @dynamicmobilitypt. We will be posting exercises to improve power throughout the month of January.
For a 1-on-1 evaluation and specific exercise plan with a trained physical therapist, call us at 720-647-3456 to get scheduled today.